 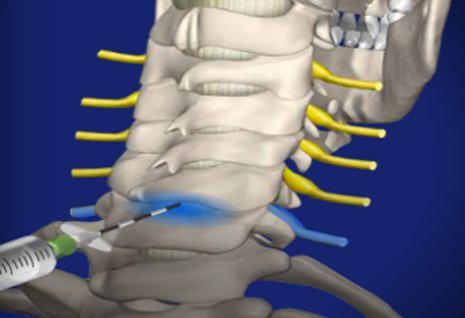 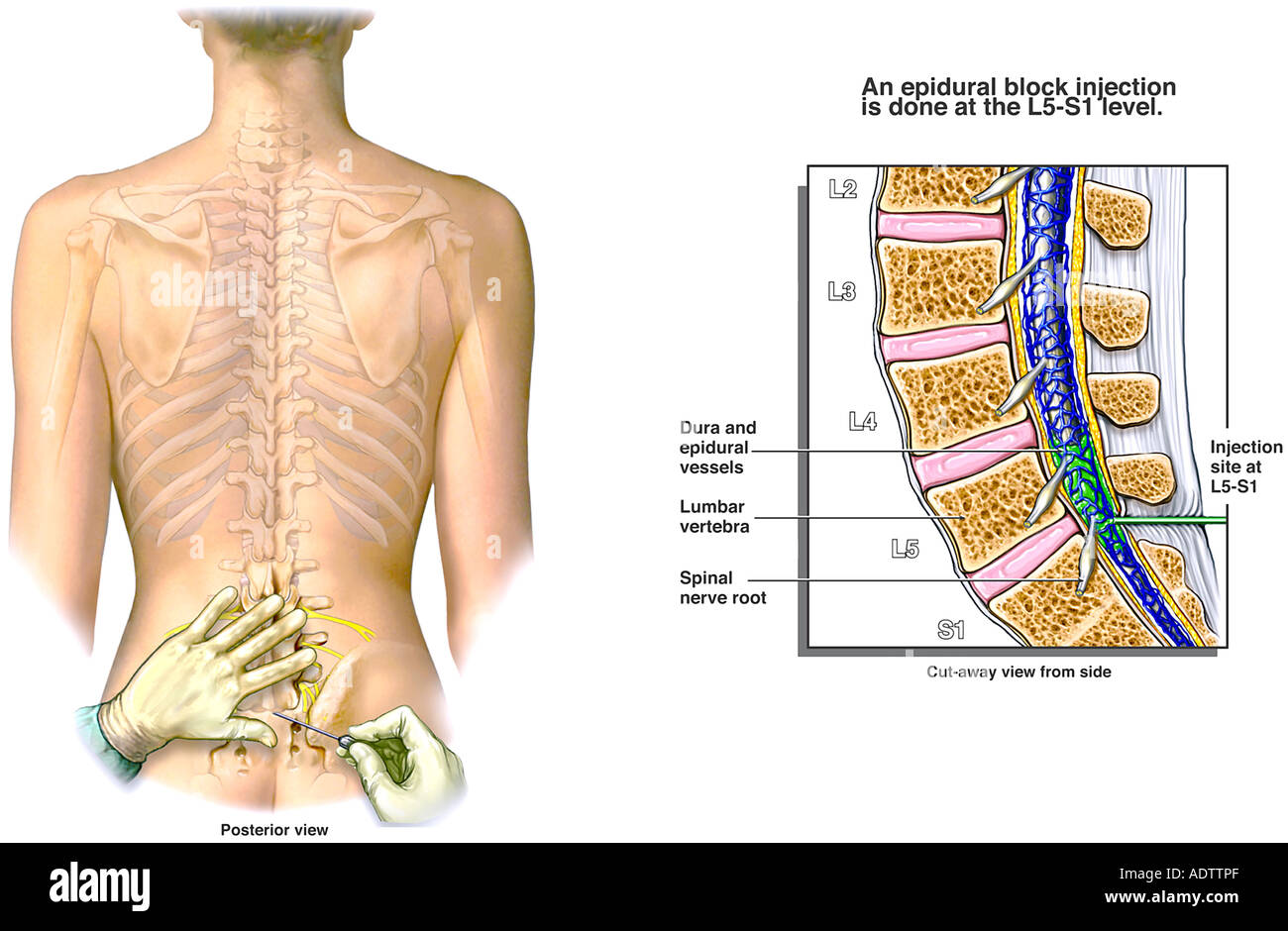
“The changes have to do with the concentration of medicine we use. The epidural a woman receives in 2023 is not the same as what has been used in years past. Ideally, the blood patch is done before a mother is discharged, but if she develops the headache after she goes home, she can return to have it done. The blood creates more buoyancy and seals the hole where the puncture occurred. McGuire explains that this is, essentially, another epidural in which blood is taken from the woman’s hand and injected into the epidural space. But the gold standard treatment for a spinal headache is what’s called an 'epidural blood patch.'”ĭr. “For treatment, we would provide over-the-counter medications or a special medication we can prescribe. It can be a sharp pain, and it feels worse when sitting up but goes away when you lie down,” she says. “The headache is either in the front or back of the head near the neck. It typically goes away on its own in a week, but sometimes it can last longer. The fluid loss affects nerves and tissues in the brain, causing a headache that usually arises within 24 hours of the epidural placement. They occur when the epidural needle goes farther than it should, and spinal fluid leaks out of the tiny hole created by the needle. “Headaches, often referred to as ‘spinal headaches,’ occur in less than 1% of all epidurals,” Dr. McGuire shares answers to common questions women have about epidurals. “And if she changes her mind later, that’s not a problem at all.”īelow, Dr. Or, if she decides to have a natural childbirth, we’ll do that, too,” she says. “If a woman chooses an epidural, we do it. McGuire, including the right to change their mind and request an epidural. The most important thing for women to know is that they have options, explains Dr. It’s primarily used during labor, but the anesthetic is also used for certain surgeries and specific causes of chronic back pain. The epidural creates a band of numbness from the belly button to the top of the legs, allowing women to stay awake and feel the pressure of labor but without the pain. The needle is removed, but the catheter remains to deliver pain medication as needed throughout labor. Used by an estimated 70-75% of women who give birth, an epidural is the most common-and most effective-type of anesthetic for pain relief during labor.Īn epidural is a numbing medicine given by inserting a needle and a catheter (a small, flexible tube) into the lower part of a woman’s back. I will answer her questions and explain any misconceptions.” Or she may have read information online that scared her about epidurals. “It might be because she wants to experience everything, including feeling what labor pain is like. “If an expectant mother says she’d like a ‘natural’ childbirth-one that doesn’t entail epidural anesthesia-I always try to honor her preferences and provide as much information as possible to help her make an informed decision,” says PJ McGuire, MD, a Yale Medicine obstetric anesthesiologist. Regardless of the specifics of their plan, when women arrive at Yale New Haven Health hospitals for delivery, an anesthesiologist is always ready to talk to them about their options. Others think an epidural is the only way to get through labor. When it’s time to have a baby, some women head to the hospital with a detailed birth plan that includes a request to avoid epidural anesthesia. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
